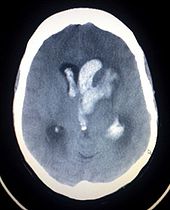
Stroke
Background Information
This content from Wikipedia has been selected by SOS Children for suitability in schools around the world. All children available for child sponsorship from SOS Children are looked after in a family home by the charity. Read more...
| Stroke | |
|---|---|
| Classification and external resources | |
| ICD- 10 | I 61- I 64 |
| ICD- 9 | 434.91 |
| OMIM | 601367 |
| DiseasesDB | 2247 |
| MedlinePlus | 000726 |
| eMedicine | neuro/9 emerg/558 emerg/557 pmr/187 |
| MeSH | D020521 |
Stroke is the rapidly developing loss of brain functions due to a disturbance in the blood vessels supplying blood to the brain. This can be due to ischemia (lack of blood supply) caused by thrombosis or embolism, or due to a hemorrhage. In medicine, a stroke, fit, or faint is sometimes referred to as an ictus [cerebri], from the Latin icere ("to strike"), especially prior to a definitive diagnosis. In the past, stroke was referred to as cerebrovascular accident or CVA, but the term "stroke" is now preferred.
Stroke is a medical emergency and can cause permanent neurological damage, complications and death if not promptly diagnosed and treated. It is the third leading cause of death in the United States. It is the leading cause of adult disability in the United States and Europe. It is the number two cause of death world-wide and may soon become the leading cause of death worldwide. Risk factors for stroke include advanced age, hypertension (high blood pressure), previous stroke or transient ischemic attack (TIA), diabetes, high cholesterol, cigarette smoking, atrial fibrillation, estrogen-containing forms of hormonal contraception, migraine with aura, and thrombophilia (a tendency to thrombosis), patent foramen ovale and several rarer disorders. High blood pressure is the most important modifiable risk factor of stroke.
The traditional definition of stroke, devised by the World Health Organization in the 1970s, is a "neurological deficit of cerebrovascular cause that persists beyond 24 hours or is interrupted by death within 24 hours". This definition was supposed to reflect the reversibility of tissue damage and was devised for the purpose, with the time frame of 24 hours being chosen arbitrarily. The 24-hour limit divides stroke from transient ischemic attack, which is a related syndrome of stroke symptoms that resolve completely within 24 hours. With the availability of treatments that, when given early, can reduce stroke severity, many now prefer alternative concepts, such as brain attack and acute ischemic cerebrovascular syndrome (modeled after heart attack and acute coronary syndrome respectively), that reflect the urgency of stroke symptoms and the need to act swiftly.
Stroke is occasionally treated with thrombolysis ("clot-buster"), but usually with supportive care ( physiotherapy and occupational therapy) and secondary prevention with antiplatelet drugs (aspirin and often dipyridamole), blood pressure control, statins and anticoagulation (in selected patients).
Classification
Strokes can be classified into two major categories: ischemic and hemorrhagic. Ischemia is due to interruption of the blood supply, while hemorrhage is due to rupture of a blood vessel or an abnormal vascular structure. 80% of strokes are due to ischemia; the remainder are due to hemorrhage.
Ischemic stroke
In an ischemic stroke, blood supply to part of the brain is decreased, leading to dysfunction and necrosis of the brain tissue in that area. There are four reasons why this might happen: thrombosis (obstruction of a blood vessel by a blood clot forming locally), embolism (idem due to an embolus from elsewhere in the body, see below), systemic hypoperfusion (general decrease in blood supply, e.g. in shock) and venous thrombosis. Stroke without an obvious explanation is termed "cryptogenic" (of unknown origin).
A widely used classification of ischemic stroke is the Bamford classification, introduced in 1991. This relies on the presenting symptoms and physical examination to identify the area of the brain affected, and can be used to predict prognosis as well as underlying etiology:
- Total anterior circulation infarct (TACI)
- Partial anterior circulation infarct (PACI)
- Lacunar infarct (LACI)
- Posterior circulation infarct (POCI)
Each of these gives a stereotypical clinical picture. Before the location of the infarction has been confirmed by diagnostic imaging (e.g. CT scan), they may be referred to as Total Anterior Circulatory Syndrome, and so on (TACS, PACS, LACS, POCS).
- Thrombotic stroke
In thrombotic stroke, a thrombus (blood clot) usually forms around atherosclerotic plaques. Since blockage of the artery is gradual, onset of symptomatic thrombotic strokes is slower. A thrombus itself (even if non-occluding) can lead to an embolic stroke (see below) if the thrombus breaks off, at which point it is called an "embolus". Thrombotic stroke can be divided into two types depending on the type of vessel the thrombus is formed on:
- Large vessel disease involves the common and internal carotids, vertebral, and the Circle of Willis. Diseases that may form thrombi in the large vessels include (in descending incidence): atherosclerosis, vasoconstriction (tightening of the artery), aortic, carotid or vertebral artery dissection, various inflammatory diseases of the blood vessel wall ( Takayasu arteritis, giant cell arteritis, vasculitis), noninflammatory vasculopathy, Moyamoya disease and fibromuscular dysplasia.
- Small vessel disease involves the smaller arteries inside the brain: branches of the circle of Willis, middle cerebral artery, stem, and arteries arising from the distal vertebral and basilar artery. Diseases that may form thrombi in the small vessels include (in descending incidence): lipohyalinosis (build-up of fatty hyaline matter in the blood vessel as a result of high blood pressure and aging) and fibrinoid degeneration (stroke involving these vessels are known as lacunar infarcts) and microatheroma (small atherosclerotic plaques).
Sickle cell anaemia, which can cause blood cells to clump up and block blood vessels, can also lead to stroke. Stroke is the second leading killer of people under 20 who suffer from sickle-cell anaemia.
- Embolic stroke
Embolic stroke refers to the blockage of an artery by an embolus, a traveling particle or debris in the arterial bloodstream originating from elsewhere. An embolus is most frequently a thrombus, but it can also be a number of other substances including fat (e.g. from bone marrow in a broken bone), air, cancer cells or clumps of bacteria (usually from infectious endocarditis).
Because an embolus arises from elsewhere, local therapy only solves the problem temporarily. Thus, the source of the embolus must be identified. Because the embolic blockage is sudden in onset, symptoms usually are maximal at start. Also, symptoms may be transient as the embolus is partially resorbed and moves to a different location or dissipates altogether.
Emboli most commonly arise from the heart (especially in atrial fibrillation) but may originate from elsewhere in the arterial tree. In paradoxical embolism, a deep vein thrombosis embolises through an atrial or ventricular septal defect in the heart into the brain.
Cardiac causes can be distinguished between high- and low-risk:
- High risk: atrial fibrillation and paroxysmal atrial fibrillation, rheumatic disease of the mitral or aortic valve disease, artificial heart valves, known cardiac thrombus of the atrium or vertricle, sick sinus syndrome, sustained atrial flutter, recent myocardial infarction, chronic myocardial infarction together with ejection fraction <28 percent, symptomatic congestive heart failure with ejection fraction <30 percent, dilated cardiomyopathy, Libman-Sacks endocarditis, Marantic endocarditis, infective endocarditis, papillary fibroelastoma, left atrial myxoma and coronary artery bypass graft (CABG) surgery
- Low risk/potential: calcification of the annulus (ring) of the mitral valve, patent foramen ovale (PFO), atrial septal aneurysm, atrial septal aneurysm with patent foramen ovale, left ventricular aneurysm without thrombus, isolated left atrial "smoke" on echocardiography (no mitral stenosis or atrial fibrillation), complex atheroma in the ascending aorta or proximal arch
- Systemic hypoperfusion
Systemic hypoperfusion is the reduction of blood flow to all parts of the body. It is most commonly due to cardiac pump failure from cardiac arrest or arrhythmias, or from reduced cardiac output as a result of myocardial infarction, pulmonary embolism, pericardial effusion, or bleeding. Hypoxemia (low blood oxygen content) may precipitate the hypoperfusion. Because the reduction in blood flow is global, all parts of the brain may be affected, especially "watershed" areas - border zone regions supplied by the major cerebral arteries. Blood flow to these areas does not necessarily stop, but instead it may lessen to the point where brain damage can occur. This phenomenon is also referred to as "last meadow" to point to the fact that in irrigation the last meadow receives the least amount of water.
- Venous thrombosis
Cerebral venous sinus thrombosis leads to stroke due to locally increased venous pressure, which exceeds the pressure generated by the arteries. Infarcts are more likely to undergo hemorrhagic transformation (leaking of blood into the damaged area) than other types of ischemic stroke.
Hemorrhagic stroke
Intracranial hemorrhage is the accumulation of blood anywhere within the skull vault. A distinction is made between intra-axial hemorrhage (blood inside the brain) and extra-axial hemorrhage (blood inside the skull but outside the brain). Intra-axial hemorrhage is due to intraparenchymal hemorrhage or intraventricular hemorrhage (blood in the ventricular system). The main types of extra-axial hemorrhage are epidural hematoma (bleeding between the dura mater and the skull), subdural hematoma (in the subdural space) and subarachnoid hemorrhage (between the arachnoid mater and pia mater). Most of the hemorrhagic stroke syndromes have specific symptoms (e.g. headache, previous head injury).
Intracerebral hemorrhage (ICH) is bleeding directly into the brain tissue, forming a gradually enlarging hematoma (pooling of blood). It generally occurs in small arteries or arterioles and is commonly due to hypertension, trauma, bleeding disorders, amyloid angiopathy, illicit drug use (e.g. amphetamines or cocaine), and vascular malformations. The hematoma enlarges until pressure from surrounding tissue limits its growth, or until it decompresses by emptying into the ventricular system, CSF or the pial surface. A third of intracerebral bleed is into the brain's ventricles. ICH has a mortality rate of 44 percent after 30 days, higher than ischemic stroke or even the very deadly subarachnoid hemorrhage.
Signs and symptoms
Stroke symptoms typically develop rapidly (seconds to minutes). The symptoms of a stroke are related to the anatomical location of the damage; nature and severity of the symptoms can therefore vary widely. Ischemic strokes usually only affect regional areas of the brain perfused by the blocked artery. Hemorrhagic strokes can affect local areas, but often can also cause more global symptoms due to bleeding and increased intracranial pressure. On the basis of the history and neurological examination, as well as the presence of risk factors, a doctor can rapidly diagnose the anatomical nature of the stroke (i.e. which part of the brain is affected), even if the exact cause is not yet known.
Pre-hospital care professionals in the United Kingdom will typically want to identify stroke risk very rapidly. If they suspect a stroke, they will typically use the Face Arm Speech Test (FAST) to assess likelihood:.
- Face - look to see if there is any drooping or loss of muscle tone on the face
- Arm - ask the patient to close their eyes and hold both arms out straight for 30 seconds - in a patient with a stroke, you might see one arm tending to slowly move down
- Speech - listen to see if you can hear any slurring of the speech not otherwise explained (e.g. alcohol) and see if they can answer simple questions (where are you?, what's your name?, what day of the week is it?)
If the area of the brain affected contains one of the three prominent Central nervous system pathways—the spinothalamic tract, corticospinal tract, and dorsal column ( medial lemniscus), symptoms may include:
- hemiplegia and muscle weakness of the face
- numbness
- reduction in sensory or vibratory sensation
In most cases, the symptoms affect only one side of the body ( unilateral). The defect in the brain is usually on the opposite side of the body (depending on which part of the brain is affected). However, the presence of any one of these symptoms does not necessarily suggest a stroke, since these pathways also travel in the spinal cord and any lesion there can also produce these symptoms.
In addition to the above CNS pathways, the brainstem also consists of the 12 cranial nerves. A stroke affecting the brainstem therefore can produce symptoms relating to deficits in these cranial nerves:
- altered smell, taste, hearing, or vision (total or partial)
- drooping of eyelid ( ptosis) and weakness of ocular muscles
- decreased reflexes: gag, swallow, pupil reactivity to light
- decreased sensation and muscle weakness of the face
- balance problems and nystagmus
- altered breathing and heart rate
- weakness in sternocleidomastoid muscle with inability to turn head to one side
- weakness in tongue (inability to protrude and/or move from side to side)
If the cerebral cortex is involved, the CNS pathways can again be affected, but also can produce the following symptoms:
- aphasia (inability to speak or understand language from involvement of Broca's or Wernicke's area)
- apraxia (altered voluntary movements)
- visual field defect
- memory deficits (involvement of temporal lobe)
- hemineglect (involvement of parietal lobe)
- disorganized thinking, confusion, hypersexual gestures (with involvement of frontal lobe)
- anosognosia (persistent denial of the existence of a, usually stroke-related, deficit)
If the cerebellum is involved, the patient may have the following:
- trouble walking
- altered movement coordination
- vertigo and or disequilibrium
Loss of consciousness, headache, and vomiting usually occurs more often in hemorrhagic stroke than in thrombosis because of the increased intracranial pressure from the leaking blood compressing on the brain.
If symptoms are maximal at onset, the cause is more likely to be a subarachnoid hemorrhage or an embolic stroke.
Pathophysiology
Ischemic stroke occurs due to a loss of blood supply to part of the brain, initiating the ischemic cascade. Brain tissue ceases to function if deprived of oxygen for more than 60 to 90 seconds and after a few hours will suffer irreversible injury possibly leading to death of the tissue, i.e., infarction. Atherosclerosis may disrupt the blood supply by narrowing the lumen of blood vessels leading to a reduction of blood flow, by causing the formation of blood clots within the vessel, or by releasing showers of small emboli through the disintegration of atherosclerotic plaques. Embolic infarction occurs when emboli formed elsewhere in the circulatory system, typically in the heart as a consequence of atria fibriliation, or in the carotid arteries. These break off, enter the cerebral circulation, then lodge in and occlude brain blood vessels.
Due to collateral circulation, within the region of brain tissue affected by ischemia there is a spectrum of severity. Thus, part of the tissue may immediately die while other parts may only be injured and could potentially recover. The ischemia area where tissue might recover is referred to as the ischemic penumbra.
As oxygen or glucose becomes depleted in ischemic brain tissue, the production of high energy phosphate compounds such as adenosine triphosphate (ATP) fails leading to failure of energy dependent processes (such as ion pumping) necessary for tissue cell survival. This sets off a series of interrelated events that result in cellular injury and death. A major cause of neuronal injury is release of the excitatory neurotransmitter glutamate. The concentration of glutamate outside the cells of the nervous system is normally kept low by so-called uptake carriers, which are powered by the concentration gradients of ions (mainly Na+) across the cell membrane. However, stroke cuts off the supply of oxygen and glucose which powers the ion pumps maintaining these gradients. As a result the transmembrane ion gradients run down, and glutamate transporters reverse their direction, releasing glutamate into the extracellular space. Glutamate acts on receptors in nerve cells (especially NMDA receptors), producing an influx of calcium which activates enzymes that digest the cells' proteins, lipids and nuclear material. Calcium influx can also lead to the failure of mitochondria, which can lead further toward energy depletion and may trigger cell death due to apoptosis.
Ischaemia also induces production of oxygen free radicals and other reactive oxygen species. These react with and damage a number of cellular and extracellular elements. Damage to the blood vessel lining or endothelium is particularly important. In fact, many antioxidant neuroprotectants such as uric acid and NXY-059 work at the level of the endothelium and not in the brain per se. Free radicals also directly initiate elements of the apoptosis cascade by means of redox signaling .
These processes are the same for any type of ischemic tissue and are referred to collectively as the ischemic cascade. However, brain tissue is especially vulnerable to ischemia since it has little respiratory reserve and is completely dependent on aerobic metabolism, unlike most other organs.
Brain tissue survival can be improved to some extent if one or more of these processes is inhibited. Drugs that scavenge Reactive oxygen species, inhibit apoptosis, or inhibit excitotoxic neurotransmitters, for example, have been shown experimentally to reduce tissue injury due to ischemia. Agents that work in this way are referred to as being neuroprotective. Until recently, human clinical trials with neuroprotective agents have failed, with the probable exception of deep barbiturate coma. However, more recently NXY-059, the disulfonyl derivative of the radical-scavenging spintrap phenylbutylnitrone, is reported be neuroprotective in stroke. This agent appears to work at the level of the blood vessel lining or endothelium. Unfortunately, after producing favorable results in one large-scale clinical trial, a second trial failed to show favorable results.
In addition to injurious effects on brain cells, ischemia and infarction can result in loss of structural integrity of brain tissue and blood vessels, partly through the release of matrix metalloproteases, which are zinc- and calcium-dependent enzymes that break down collagen, hyaluronic acid, and other elements of connective tissue. Other proteases also contribute to this process. The loss of vascular structural integrity results in a breakdown of the protective blood brain barrier that contributes to cerebral edema, which can cause secondary progression of the brain injury.
As is the case with any type of brain injury, the immune system is activated by cerebral infarction and may under some circumstances exacerbate the injury caused by the infarction. Inhibition of the inflammatory response has been shown experimentally to reduce tissue injury due to cerebral infarction, but this has not proved out in clinical studies.
Hemorrhagic strokes result in tissue injury by causing compression of tissue from an expanding hematoma or hematomas. This can distort and injure tissue. In addition, the pressure may lead to a loss of blood supply to affected tissue with resulting infarction, and the blood released by brain hemorrhage appears to have direct toxic effects on brain tissue and vasculature.
Diagnosis
Stroke is diagnosed through several techniques: a neurological examination, CT scans (most often without contrast enhancements) or MRI scans, Doppler ultrasound, and arteriography. The diagnosis of stroke itself is clinical, with assistance from the imaging techniques. Imaging techniques also assist in determining the subtypes and cause of stroke. There is yet no commonly used blood test for the stroke diagnosis itself, though blood tests may be of help in finding out the likely cause of stroke.
Physical examination
A systematic review found that acute facial paresis, arm drift, or abnormal speech are the best findings.
Imaging
For diagnosing ischemic stroke in the emergency setting:
- CT scans (without contrast enhancements)
- sensitivity= 16%
- specificity= 96%
- MRI scan
- sensitivity= 83%
- specificity= 98%
For diagnosing hemorrhagic stroke in the emergency setting:
- CT scans (without contrast enhancements)
- sensitivity= 89%
- specificity= 100%
- MRI scan
- sensitivity= 81%
- specificity= 100%
For detecting chronic hemorrhages, MRI scan is more sensitive.
For the assessment of stable stroke, nuclear medicine scans SPECT and PET/CT may be helpful. SPECT documents cerebral blood flow and PET with FDG isotope the metabolic activity of the neurons.
Underlying etiology
When a stroke has been diagnosed, various other studies may be performed to determine the underlying etiology. With the current treatment and diagnosis options available, it is of particular importance to determine whether there is a peripheral source of emboli. Test selection may vary, since the cause of stroke varies with age, comorbidity and the clinical presentation. Commonly used techniques include:
- an ultrasound/doppler study of the carotid arteries (to detect carotid stenosis) or dissection of the precerebral arteries
- an electrocardiogram (ECG) and echocardiogram (to identify arrhythmias and resultant clots in the heart which may spread to the brain vessels through the bloodstream)
- a Holter monitor study to identify intermittent arrhythmias
- an angiogram of the cerebral vasculature (if a bleed is thought to have originated from an aneurysm or arteriovenous malformation)
- blood tests to determine hypercholesterolemia, bleeding diathesis and some rarer causes such as homocysteinuria
Prevention
Given the disease burden of stroke, prevention is an important public health concern. Primary prevention is a lot less effective than secondary prevention (as judged by the number needed to treat to prevent one stroke per year). Recent guidelines detail the evidence for primary prevention in stroke. Because stroke may indicate underlying atherosclerosis, it is important to determine the patient's risk for other cardiovascular diseases such as coronary heart disease. Conversely, aspirin prevents against first stroke in patients who have suffered a myocardial infarction.
The most important modifiable risk factors for stroke are high blood pressure and atrial fibrillation. Other modifiable risk factors include high blood cholesterol levels, diabetes, cigarette smoking (active and passive), heavy alcohol consumption and drug use, lack of physical activity, obesity and unhealthy diet. Alcohol use could predispose to ischemic stroke, and intracerebral and subarachnoid hemorrhage via multiple mechanisms (for example via hypertension, atrial fibrillation, rebound thrombocytosis and platelet aggregation and clotting disturbances). The drugs most commonly associated with stroke are cocaine, amphetamines causing hemorrhagic stroke, but also over-the-counter cough and cold drugs containing sympathomimetics.
No high quality studies have shown the effectiveness of interventions aimed at weight reduction, promotion of regular exercise, reducing alcohol consumption or smoking cessation. Nonetheless, given the large body of circumstantial evidence, best medical management for stroke includes advise on diet, exercise, smoking and alcohol use. Medication or drug therapy is the most common method of stroke prevention; carotid endarterectomy can be a useful surgical method of preventing stroke.
- Blood pressure
Hypertension accounts for 35-50% of stroke risk. Epidemiological studies suggest that even a small blood pressure reduction (5 to 6 mmHg systolic, 2 to 3 mmHg diastolic) would result in 40% fewer strokes. Lowering blood pressure has been conclusively shown to prevent both ischemic and hemorrhagic strokes. It is equally important in secondary prevention. Even patients older than 80 years and those with isolated systolic hypertension benefit from antihypertensive therapy. Studies show that intensive antihypertensive therapy results in a greater risk reduction. The available evidence does not show large differences in stroke prevention between antihypertensive drugs —therefore, other factors such as protection against other forms of cardiovascular disease should be considered and cost.
- Atrial fibrillation
Patients with atrial fibrillation have a risk of 5% each year to develop stroke, and this risk is even higher in those with valvular atrial fibrillation. Depending on the stroke risk, anticoagulation with medications such as coumarins or aspirin is warranted for stroke prevention.
- Blood lipids
High cholesterol levels have been inconsistently associated with (ischemic) stroke. Statins have been shown to reduce the risk of stroke by about 15%. Since earlier meta-analyses of other lipid-lowering drugs did not show a decreased risk, statins might exert there effect through mechanisms other than their lipid-lowering effects.
- Diabetes mellitus
Patients with diabetes mellitus are 2 to 3 times more likely to develop stroke, and they commonly have hypertension and hyperlipidemia. Intensive disease control has been shown to reduce microvascular complications such as nephropathy and retinopathy but not macrovascular complications such as stroke.
- Anticoagulation drugs
Aspirin or other antiplatelet drugs are highly effective in secondary prevention after a stroke or transient ischemic attack. Low doses of aspirin (for example 75-150 mg) are as effective as high doses but have fewer side-effects; the lowest effective dose remains unknown. Thienopyridines ( clopidogrel, ticlopidine) are modestly more effective than aspirin and have a decreased risk of gastrointestinal bleeding, but they are more expensive. Their exact role remains controversial. Ticlopidine has more skin rash, diarrhea, neutropenia and thrombotic thrombocytopenic purpura. Dipyridamole can be added to aspirin therapy to provide a small additional benefit, even though headache is a common side-effect. Low-dose aspirin is also effective for stroke prevention after sustaining a myocardial infarction. Oral anticoagulants are not advised for stroke prevention —any benefit is offset by bleeding risk.
In primary prevention however, antiplatelet drugs did not reduce the risk of ischemic stroke while increasing the risk of major bleeding. Further studies are needed to investigate a possible protective effect of aspirin against ischemic stroke in women.
- Surgery
Surgical procedures such as carotid endarterectomy or carotid angioplasty can be used to remove significant atherosclerotic narrowing (stenosis) of the carotid artery, which supplies blood to the brain. There is a large body of evidence supporting this procedure in selected cases. Endarterectomy for a significant stenosis has been shown to be useful in the secondary prevention after a previous symptomatic stroke. Carotid artery stenting has not been shown to be equally useful. Patients are selected for surgery based on age, gender, degree of stenosis, time since symptoms and patients' preferences. Surgery is most efficient when not delayed too long —the risk of recurrent stroke in a patient who has a 50% or greater stenosis is up to 20% after 5 years, but endarterectomy reduces this risk to around 5%. The number of procedures needed to cure one patient was 5 for early surgery (within two weeks after the initial stroke), but 125 if delayed longer than 12 weeks.
Screening for carotid artery narrowing has not been shown to be a useful screening test in the general population. Studies of surgical intervention for carotid artery stenosis without symptoms have shown only a small decrease in the risk of stroke. To be beneficial, the complication rate of the surgery should be kept > 4%. Even then, for 100 surgeries, 5 patients will benefit by avoiding stroke, 3 will develop stroke despite surgery, 3 will develop stroke or die due to the surgery itself, and 89 will remain stroke-free but would also have done so without intervention.
- Nutritional and metabolic interventions
Nutrition, specifically the Mediterranean-style diet, has the potential of more than halving stroke risk.
With regards to lowering homocysteine, a meta-analysis of previous trials has concluded that lowering homocysteine with folic acid and other supplements may reduce stroke risk. However, the two largest randomized controlled trials included in the meta-analysis had conflicting results. One reported positve results; whereas the other was negative.
Treatment
Early assessment
Early recognition of the signs of stroke is generally regarded as important. Only detailed physical examination and medical imaging provide information on the presence, type, and extent of stroke, and hence hospital attendance — even if the symptoms were brief — is advised.
Studies show that patients treated in hospitals with a dedicated Stroke Team or Stroke Unit and a specialized care program for stroke patients have improved odds of recovery.
Ischemic stroke
An ischemic stroke is due to a thrombus (blood clot) occluding a cerebral artery, a patient is given antiplatelet medication (aspirin, clopidogrel, dipyridamole), or anticoagulant medication ( warfarin), dependent on the cause, when this type of stroke has been found. Hemorrhagic stroke must be ruled out with medical imaging, since this therapy would be harmful to patients with that type of stroke.
Whether thrombolysis is performed or not, the following investigations are required:
- Stroke symptoms are documented, often using scoring systems such as the National Institutes of Health Stroke Scale, the Cincinnati Stroke Scale, and the Los Angeles Prehospital Stroke Screen. The Cincinnati Stroke Scale is used by emergency medical technicians (EMTs) to determine whether a patient needs transport to a stroke centre.
- A CT scan is performed to rule out hemorrhagic stroke
- Blood tests, such as a full blood count, coagulation studies ( PT/INR and APTT), and tests of electrolytes, renal function, liver function tests and glucose levels are carried out.
Other immediate strategies to protect the brain during stroke include ensuring that blood sugar is as normal as possible (such as commencement of an insulin sliding scale in known diabetics), and that the stroke patient is receiving adequate oxygen and intravenous fluids. The patient may be positioned so that his or her head is flat on the stretcher, rather than sitting up, since studies have shown that this increases blood flow to the brain. Additional therapies for ischemic stroke include aspirin (50 to 325 mg daily), clopidogrel (75 mg daily), and combined aspirin and dipyridamole extended release (25/200 mg twice daily).
It is common for the blood pressure to be elevated immediately following a stroke. Studies indicated that while high blood pressure causes stroke, it is actually beneficial in the emergency period to allow better blood flow to the brain.
If studies show carotid stenosis, and the patient has residual function in the affected side, carotid endarterectomy (surgical removal of the stenosis) may decrease the risk of recurrence if performed rapidly after stroke.
If the stroke has been the result of cardiac arrhythmia with cardiogenic emboli, treatment of the arrhythmia and anticoagulation with warfarin or high-dose aspirin may decrease the risk of recurrence. Stroke prevention treatment for a common arrhythmia, atrial fibrillation, is determined according to the CHADS/CHADS2 system.
Therapeutic hypothermia
Most of the data concerning therapeutic hypothermia’s effectiveness in treating ischemic stroke is limited to animal studies. These studies have focused primarily on ischemic as opposed to hemorrhagic stroke, as hypothermia has been associated with a lower clotting threshold. In these animal studies investigating the effect of temperature decline following ischemic stroke, hypothermia has been shown to be an effective all purpose neuroprotectant.This promising data has lead to the initiation of a variety of human studies. Unfortunately, at the time of this article’s publishing, this research have yet to return results. However, in terms of feasibility, the use of hypothermia to control intracranial pressure (ICP) after an ischemic stroke was found to be both safe and practical. The device used in this study was called the Arctic Sun
Thrombolysis
In increasing numbers of primary stroke centers, pharmacologic thrombolysis ("clot busting") with the drug tissue plasminogen activator (tPA), is used to dissolve the clot and unblock the artery. However, the use of tPA in acute stroke is controversial. On one hand, it is endorsed by the American Heart Association and the American Academy of Neurology as the recommended treatment for acute stroke within three hours of onset of symptoms as long as there are not other contraindications (such as abnormal lab values, high blood pressure, or recent surgery). This position for tPA is based upon the findings of two studies by one group of investigators which showed that tPA improves the chances for a good neurological outcome. When administered within the first three hours, 39% of all patients who were treated with tPA had a good outcome at three months, only 26% of placebo controlled patients had a good functional outcome. However, in the NINDS trial 6.4% of patients with large strokes developed substantial brain hemorrhage as a complication from being given tPA. tPA is often misconstrued as a "magic bullet" and it is important for patients to be aware that despite the study that supports its use, some of the data were flawed and the safety and efficacy of tPA is controversial. A recent study found the mortality to be higher among patients receiving tPA versus those who did not. Additionally, it is the position of the American Academy of Emergency Medicine that objective evidence regarding the efficacy, safety, and applicability of tPA for acute ischemic stroke is insufficient to warrant its classification as standard of care. Until additional evidence clarifies such controversies, physicians are advised to use their discretion when considering its use. Given the cited absence of definitive evidence, AAEM believes it is inappropriate to claim that either use or non-use of intravenous thrombolytic therapy constitutes a standard of care issue in the treatment of stroke.
Mechanical thrombectomy
Another intervention for acute ischemic stroke is removal of the offending thrombus directly. This is accomplished by inserting a catheter into the femoral artery, directing it into the cerebral circulation, and deploying a corkscrew-like device to ensnare the clot, which is then withdrawn from the body. In August 2004, based on data from the MERCI (Mechanical Embolus Removal in Cerebral Ischemia) Trial, the FDA cleared several of these devices, called the Merci X5 and X6 Retrievers. The newer generation Merci L5 Retriever was additionally used in the Multi MERCI trial. Both the MERCI and Multi MERCI trials required the first pass with the Merci Retriever to be initiated within 8 hours of onset of symptoms.
Embolic stroke
Anticoagulation can prevent recurrent stroke. Among patients with nonvalvular atrial fibrillation, anticoagulation can reduce stroke by 60% while antiplatelet agents can reduce stroke by 20%.. However, a recent meta-analysis suggests harm from anti-coagulation started early after an embolic stroke.
Hemorrhagic stroke
Patients with bleeding into ( intracerebral hemorrhage) or around the brain (subarachnoid hemorrhage), require neurosurgical evaluation to detect and treat the cause of the bleeding. Anticoagulants and antithrombotics, key in treating ischemic stroke, can make bleeding worse and cannot be used in intracerebral hemorrhage. Patients are monitored and their blood pressure, blood sugar, and oxygenation are kept at optimum levels.
Care and rehabilitation
Stroke rehabilitation is the process by which patients with disabling strokes undergo treatment to help them return to normal life as much as possible by regaining and relearning the skills of everyday living. It also aims to help the survivor understand and adapt to difficulties, prevent secondary complications and educate family members to play a supporting role.
A rehabilitation team is usually multidisciplinary as it involves staff with different skills working together to help the patient. These include nursing staff, physiotherapy, occupational therapy, speech and language therapy, and usually a physician trained in rehabilitation medicine. Some teams may also include psychologists, social workers, and pharmacists since at least one third of the patients manifest post stroke depression. Validated instruments such as the Barthel scale may be used to assess the likelihood of a stroke patient being able to manage at home with or without support subsequent to discharge from hospital.
Good nursing care is fundamental in maintaining skin care, feeding, hydration, positioning, and monitoring vital signs such as temperature, pulse, and blood pressure. Stroke rehabilitation begins almost immediately.
For most stroke patients, physical therapy (PT) and occupational therapy (OT) are the cornerstones of the rehabilitation process. Often, assistive technology such as a wheelchair, walkers, canes, and orthosis may be beneficial. PT and OT have overlapping areas of working but their main attention fields are; PT involves re-learning functions as transferring, walking and other gross motor functions. OT focusses on exercises and training to help relearn everyday activities known as the Activities of daily living (ADLs) such as eating, drinking, dressing, bathing, cooking, reading and writing, and toileting. Speech and language therapy is appropriate for patients with problems understanding speech or written words, problems forming speech and problems with eating (swallowing).
Patients may have particular problems, such as complete or partial inability to swallow, which can cause swallowed material to pass into the lungs and cause aspiration pneumonia. The condition may improve with time, but in the interim, a nasogastric tube may be inserted, enabling liquid food to be given directly into the stomach. If swallowing is still unsafe after a week, then a percutaneous endoscopic gastrostomy (PEG) tube is passed and this can remain indefinitely.
Stroke rehabilitation should be started as immediately as possible and can last anywhere from a few days to over a year. Most return of function is seen in the first few days and weeks, and then improvement falls off with the "window" considered officially by U.S. state rehabilitation units and others to be closed after six months, with little chance of further improvement. However, patients have been known to continue to improve for years, regaining and strengthening abilities like writing, walking, running, and talking. Daily rehabilitation exercises should continue to be part of the stroke patient's routine. Complete recovery is unusual but not impossible and most patients will improve to some extent : a correct diet and exercise are known to help the brain to self-recover.
Prognosis
Disability affects 75% of stroke survivors enough to decrease their employability. Stroke can affect patients physically, mentally, emotionally, or a combination of the three. The results of stroke vary widely depending on size and location of the lesion. Dysfunctions correspond to areas in the brain that have been damaged.
Some of the physical disabilities that can result from stroke include paralysis, numbness, pressure sores, pneumonia, incontinence, apraxia (inability to perform learned movements), difficulties carrying out daily activities, appetite loss, speech loss, vision loss, and pain. If the stroke is severe enough, or in a certain location such as parts of the brainstem, coma or death can result.
Emotional problems resulting from stroke can result from direct damage to emotional centers in the brain or from frustration and difficulty adapting to new limitations. Post-stroke emotional difficulties include anxiety, panic attacks, flat affect (failure to express emotions), mania, apathy, and psychosis.
30 to 50% of stroke survivors suffer post stroke depression, which is characterized by lethargy, irritability, sleep disturbances, lowered self esteem, and withdrawal. Depression can reduce motivation and worsen outcome, but can be treated with antidepressants.
Emotional lability, another consequence of stroke, causes the patient to switch quickly between emotional highs and lows and to express emotions inappropriately, for instance with an excess of laughing or crying with little or no provocation. While these expressions of emotion usually correspond to the patient's actual emotions, a more severe form of emotional lability causes patients to laugh and cry pathologically, without regard to context or emotion. Some patients show the opposite of what they feel, for example crying when they are happy. Emotional lability occurs in about 20% of stroke patients.
Cognitive deficits resulting from stroke include perceptual disorders, speech problems, dementia, and problems with attention and memory. A stroke sufferer may be unaware of his or her own disabilities, a condition called anosognosia. In a condition called hemispatial neglect, a patient is unable to attend to anything on the side of space opposite to the damaged hemisphere.
Up to 10% of all stroke patients develop seizures, most commonly in the week subsequent to the event; the severity of the stroke increases the likelihood of a seizure.
Epidemiology
Stroke could soon be the most common cause of death worldwide. Stroke is the third leading cause of death in the Western world, after heart disease and cancer, and causes 10% of deaths worldwide.
The incidence of stroke increases exponentially from 30 years of age, and etiology varies by age. Advanced age is one of the most significant stroke risk factors. 95% of strokes occur in people age 45 and older, and two-thirds of strokes occur in those over the age of 65. A person's risk of dying if he or she does have a stroke also increases with age. However, stroke can occur at any age, including in fetuses.
Family members may have a genetic tendency for stroke or share a lifestyle that contributes to stroke. Higher levels of Von Willebrand factor are more common amongst people who have had ischemic stroke for the first time. The results of this study found that the only significant genetic factor was the person's blood type. Having had a stroke in the past greatly increases one's risk of future strokes.
Men are 1.25 times more likely to suffer strokes than women, yet 60% of deaths from stroke occur in women. Since women live longer, they are older on average when they have their strokes and thus more often killed (NIMH 2002). Some risk factors for stroke apply only to women. Primary among these are pregnancy, childbirth, menopause and the treatment thereof ( HRT).
History
Hippocrates (460 to 370 BC) was first to describe the phenomenon of sudden paralysis. Apoplexy, from the Greek word meaning "struck down with violence,” first appeared in Hippocratic writings to describe this phenomenon.
The word stroke was used as a synonym for apoplectic seizure as early as 1599, and is a fairly literal translation of the Greek term.
In 1658, in his Apoplexia, Johann Jacob Wepfer (1620–1695) identified the cause of hemorrhagic stroke when he suggested that people who had died of apoplexy had bleeding in their brains. Wepfer also identified the main arteries supplying the brain, the vertebral and carotid arteries, and identified the cause of ischemic stroke when he suggested that apoplexy might be caused by a blockage to those vessels.
Rudolf Virchow first described the mechanism of thromboembolism as a major factor.